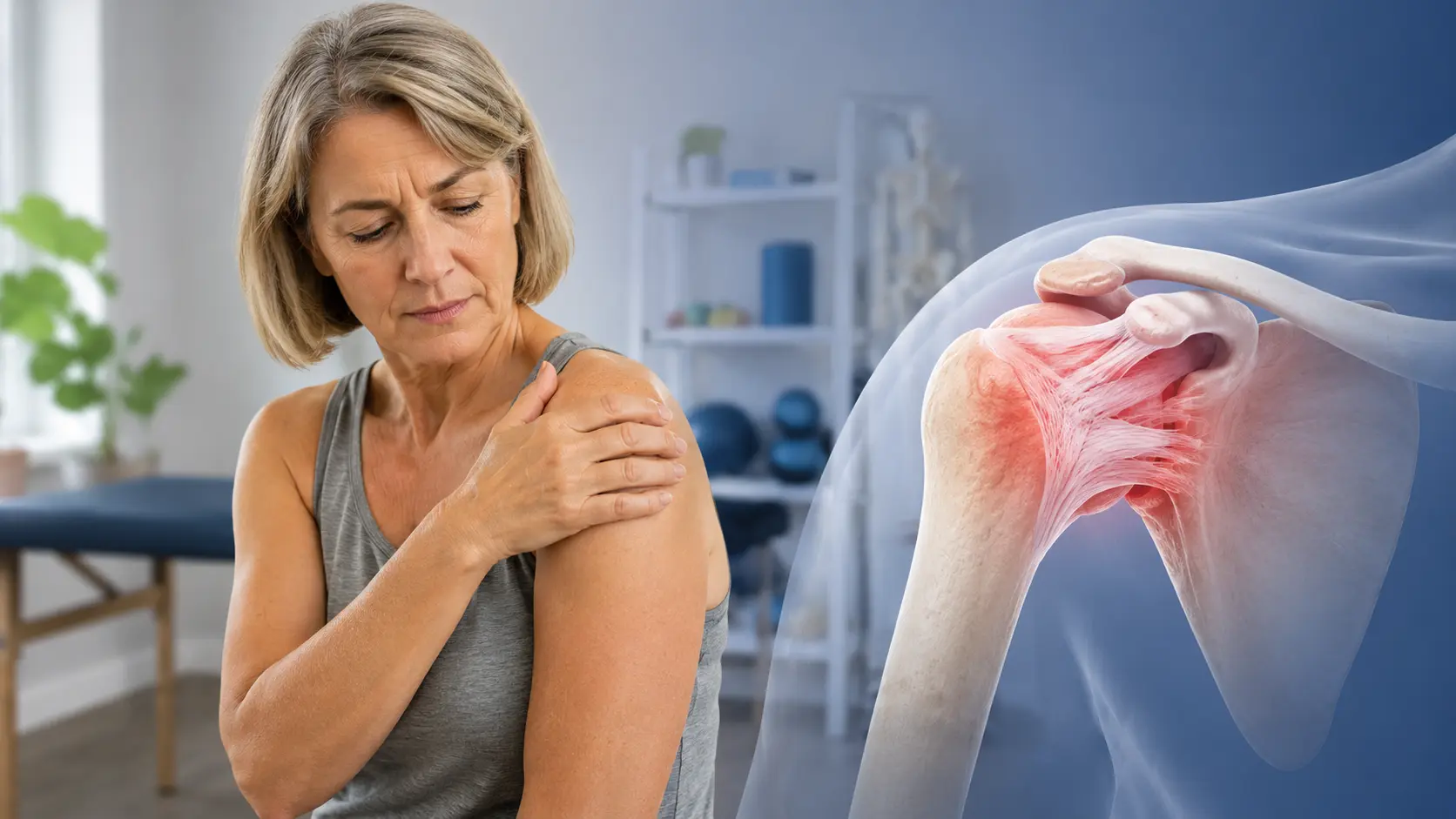

Frozen shoulder, also known as adhesive capsulitis, is a painful and frustrating condition that can severely limit movement in the shoulder joint. Many people are surprised by how long recovery can take, with symptoms sometimes lasting more than a year. Everyday tasks such as getting dressed, reaching overhead, driving, or even sleeping comfortably can become difficult during this time.
Unlike a simple muscle strain or minor injury, frozen shoulder develops gradually and often follows a slow healing process. The condition involves inflammation and tightening of the shoulder capsule, leading to pain, stiffness, and restricted movement. Understanding the stages of frozen shoulder and the available treatment options can help patients feel more prepared during recovery.
Frozen shoulder occurs when the connective tissue surrounding the shoulder joint becomes inflamed and thickened. Over time, the capsule tightens and forms scar-like tissue, making movement increasingly difficult.
The exact cause is not always clear, but frozen shoulder is more common in people aged between 40 and 60 years and tends to affect women more frequently than men. It can also develop after shoulder injuries, surgery, or long periods of immobility.
Certain health conditions may increase the risk, including:
The condition usually affects one shoulder, although some people may eventually develop symptoms in the opposite shoulder.
One of the main reasons frozen shoulder takes so long to resolve is because the condition progresses through several distinct stages. Each stage can last for months, and recovery often depends on how severely the shoulder capsule has tightened.
The healing process is gradual because the body needs time to reduce inflammation, soften scar tissue, and restore joint mobility. Unlike a broken bone that follows a more predictable healing timeline, frozen shoulder involves changes in soft tissues that recover slowly.
Pain may settle before movement returns fully, which can make recovery feel inconsistent or unpredictable. Some patients improve steadily, while others experience periods where progress seems to stall.
This is the early and often most painful stage.
During the freezing stage, shoulder pain gradually worsens over time. Movement becomes increasingly limited, especially when reaching overhead or behind the back. Pain is often worse at night and may interfere with sleep.
Common symptoms include:
This stage may last anywhere from 6 weeks to 9 months.
During the frozen stage, pain may begin to improve, but stiffness becomes more severe.
Many people notice that while the shoulder hurts less, they are unable to move it properly. Activities such as fastening a bra, reaching into cupboards, or putting on a jacket can become extremely difficult.
Symptoms during this stage include:
The frozen stage commonly lasts between 4 and 12 months.
The thawing stage is when recovery gradually begins.
Shoulder movement slowly improves, and pain continues to decrease. While this stage is encouraging, improvement can still be slow and may continue for many months.
Recovery during the thawing stage often includes:
This stage may last from 6 months to 2 years depending on the severity of the condition.
Diagnosis is usually based on symptoms, medical history, and physical examination. A doctor or shoulder specialist will assess range of motion and determine whether stiffness is affecting both active and passive movement.
Imaging tests may sometimes be recommended to rule out other conditions such as arthritis or rotator cuff tears.
These investigations may include:
Early diagnosis can help guide treatment and prevent unnecessary worsening of stiffness.
Treatment aims to reduce pain, improve movement, and support gradual recovery. Because frozen shoulder often resolves slowly, treatment plans may vary depending on the stage of the condition and the severity of symptoms.
Pain relief is often one of the first priorities, especially during the freezing stage.
Treatment may include:
Managing pain can help patients maintain some level of shoulder movement and avoid further stiffness.
Physiotherapy plays an important role in frozen shoulder recovery. A physiotherapist can guide safe exercises designed to improve flexibility and restore range of motion gradually.
Treatment may involve:
Exercises should be gentle and progressive, as overly aggressive stretching can sometimes worsen pain.
Corticosteroid injections may help reduce inflammation and pain, particularly in the early stages.
Some patients experience temporary improvement in pain and movement after injections, allowing them to participate more comfortably in physiotherapy.
The effectiveness of injections can vary depending on the stage of the condition.
Hydrodilatation is a procedure where sterile fluid is injected into the shoulder joint to stretch the capsule gently.
This treatment may help improve movement and reduce stiffness in some patients. It is often performed under imaging guidance to ensure accurate placement.
Surgery is usually considered only when symptoms remain severe despite non-surgical treatment.
Options may include:
These procedures aim to improve movement by releasing tight tissue around the shoulder joint.
Surgery is generally reserved for patients with persistent stiffness and significant loss of function.
In some cases, frozen shoulder may gradually improve without surgery. However, recovery can take a long time, and some people may continue to experience lingering stiffness or reduced movement even after symptoms settle.
Early treatment may help improve comfort and maintain mobility during the recovery process.
Ignoring symptoms completely may lead to worsening stiffness and prolonged limitations in shoulder function.
Living with frozen shoulder can be physically and emotionally challenging, especially when recovery feels slow. The following strategies may help support day-to-day comfort and function:
Patience is important, as recovery often occurs gradually over many months.
It is important to seek medical assessment if shoulder pain and stiffness are interfering with daily life or worsening over time.
You should also seek medical advice if you experience:
Early assessment can help confirm the diagnosis and rule out other shoulder conditions.
Every patient’s recovery timeline is different. Some people regain nearly full shoulder movement, while others may continue to notice mild stiffness long-term.
Factors that may influence recovery include:
Although frozen shoulder can be frustratingly slow to improve, many patients eventually experience meaningful pain relief and functional recovery with appropriate management.
Frozen shoulder can last anywhere from 12 months to 3 years depending on the severity of the condition and the stage at which treatment begins.
Most people improve over time, although some may continue to experience mild stiffness or reduced range of motion long-term.
There is no instant cure, but early physiotherapy, pain management, and appropriate medical treatment may help improve recovery and maintain shoulder mobility.
Overly aggressive or painful exercises can sometimes increase inflammation and discomfort. Gentle, guided stretching is usually recommended.
MRI scans may show thickening of the shoulder capsule and inflammation, but diagnosis is often based primarily on symptoms and physical examination.
Most patients improve without surgery. Surgical treatment is generally reserved for severe cases that do not respond to conservative management.
=====