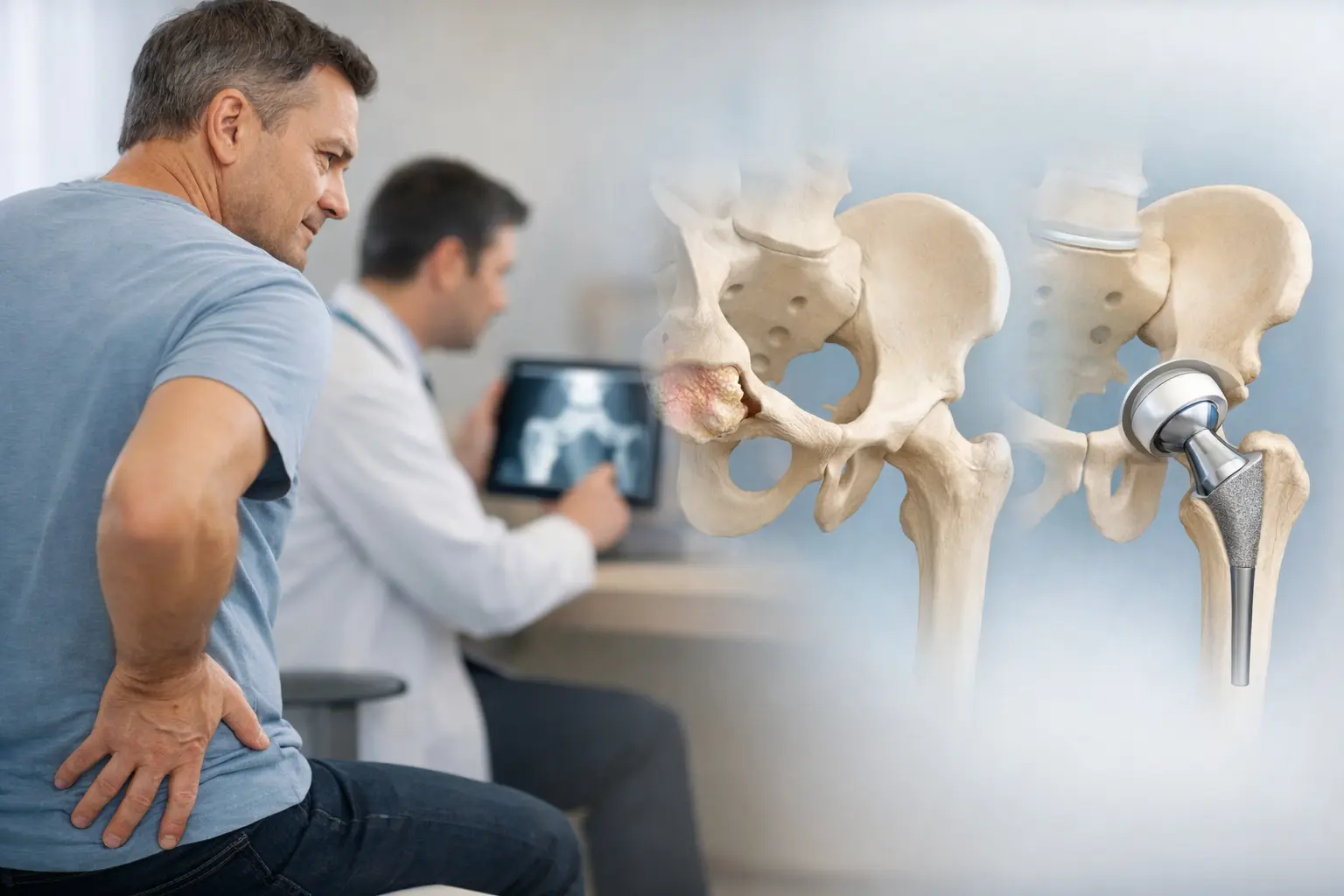

Avascular necrosis (AVN), also known as osteonecrosis, is a condition where the blood supply to the bone is disrupted, leading to bone death and eventual joint collapse. When it affects the hip, it can progress quickly and often results in significant pain, reduced mobility, and loss of quality of life.
While hip replacement is a well-established treatment for advanced joint damage, hip replacement for AVN is quite different from procedures performed for osteoarthritis or other degenerative conditions. Understanding these differences can help patients feel more informed and confident about their treatment journey.
AVN typically affects younger and more active individuals compared to those undergoing hip replacement for osteoarthritis. It can be linked to factors such as:
What makes AVN particularly challenging is its unpredictable and often rapid progression. In many cases, the condition advances silently until the bone begins to collapse.
One of the defining features of AVN is how quickly it can worsen.
Unlike osteoarthritis, which develops gradually over years, AVN can progress within months. Patients may go from mild discomfort to severe pain in a relatively short period.
Key characteristics of AVN progression include:
Because of this accelerated progression, early diagnosis is critical. However, once the femoral head (the ball of the hip joint) begins to collapse, joint-preserving treatments are often no longer effective, and hip replacement becomes the most reliable option.
Hip replacement surgery for AVN requires a more tailored approach compared to standard cases.
In AVN, the bone may already be weakened or partially collapsed. Surgeons must carefully assess:
This influences implant selection and positioning.
Many AVN patients are younger (often in their 30s to 50s), which introduces additional considerations:
Surgeons often choose implants designed for longevity and stability, such as:
Because AVN may distort the normal anatomy of the hip, surgeons may need to:
The good news is that outcomes for hip replacement in AVN patients are generally very positive—especially with modern surgical techniques and implant technology.
However, there are some differences worth noting.
Most patients experience:
These outcomes are comparable to those seen in osteoarthritis patients.
Because AVN patients are often younger and more active:
That said, advances in materials have significantly improved implant lifespan.
Recovery is typically similar to other hip replacements, but younger patients may:
Some AVN-specific considerations include:
Even though hip replacement is highly effective, timing remains important.
Early-stage AVN may be treated with joint-preserving procedures such as core decompression. However, once collapse occurs, delaying surgery can lead to:
Seeking specialist advice early ensures the best possible outcome and helps determine the most appropriate treatment pathway.
Most patients return to a highly functional and active lifestyle after surgery.
Common improvements include:
Patients are usually advised to avoid high-impact sports to prolong the life of the implant.
Long-term success depends on:
Visual Direction: Clean, modern, and clinical with a human touch
Scene Concept:
Colour Palette:
Mood:
Composition:
Avascular necrosis is a condition where reduced blood supply causes bone tissue in the hip to die, leading to joint collapse if untreated.
AVN progresses more rapidly and is caused by loss of blood supply, whereas osteoarthritis develops slowly due to wear and tear of the joint.
Hip replacement is usually recommended once the femoral head has collapsed or when pain and function significantly affect daily life.
Yes, most patients experience excellent pain relief and improved mobility. Outcomes are comparable to other types of hip replacement.
Yes, AVN often affects people in their 30s to 50s, which is younger than the typical osteoarthritis patient.
Because AVN patients are often younger, there is a higher chance of needing a revision later in life. However, modern implants are designed to last many years.
Most patients resume normal activities within 6–12 weeks, with continued improvement over several months.