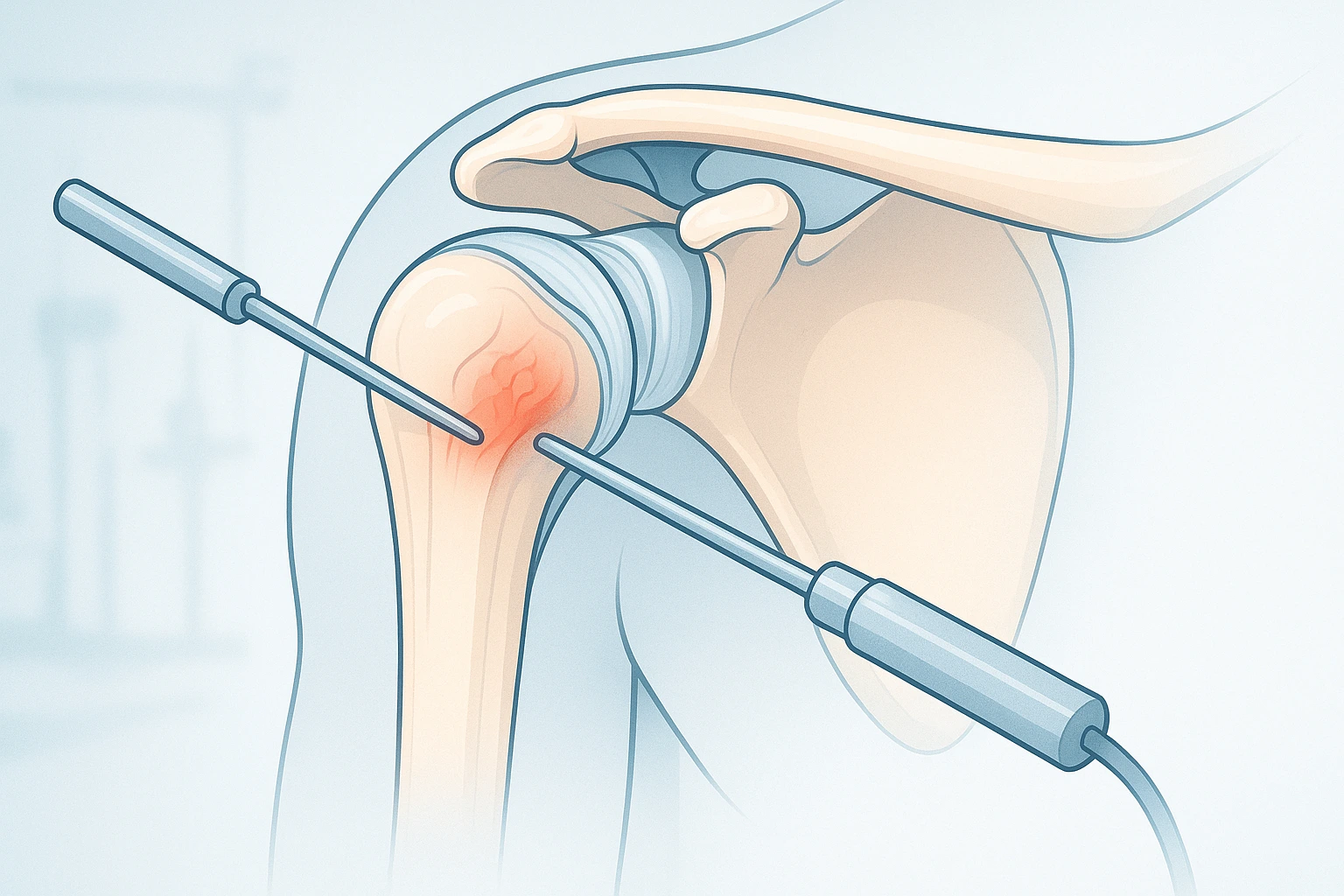

Shoulder arthroscopy is a minimally invasive surgical procedure where a surgeon inserts a small camera (arthroscope) into the shoulder joint through tiny incisions. Special instruments allow them to repair damaged tissue without opening the joint fully.
Because arthroscopy is less invasive than traditional surgery, it typically results in:
It is a powerful option for patients whose shoulder problems involve treatable soft-tissue or structural damage rather than severe joint deterioration.
Shoulder replacement (arthroplasty) is a major operation where damaged parts of the shoulder joint are removed and replaced with artificial components. It is usually recommended for advanced degeneration, severe arthritis, complex fractures, or when pain is constant and function is significantly impaired.
Although shoulder replacement can dramatically improve quality of life, it comes with:
Because of this, doctors often consider arthroscopy first—if the underlying problem can be corrected without replacing the joint.
You may be a stronger candidate for arthroscopy over a replacement if:
1. Your cartilage is still in good condition.
Arthroscopy works best when the joint surfaces are not severely worn down by osteoarthritis.
2. Your symptoms come from soft-tissue damage rather than bone-on-bone degeneration.
Many shoulder problems arise from torn tendons, damaged cartilage rings, or inflammation—conditions arthroscopy can effectively treat.
3. You’re active and wish to return to sport or manual work.
Arthroscopy allows a more natural joint to be preserved, which is beneficial for strength, mobility, and long-term activity levels.
4. You’re younger and want to avoid early shoulder replacement.
Joint replacements don’t last forever. Younger patients risk needing multiple revision surgeries later in life. Arthroscopy preserves natural anatomy, delaying or avoiding replacement altogether.
5. Pain is moderate to severe but does not limit all daily activities.
If your shoulder still moves reasonably well but hurts during specific activities, arthroscopy may be ideal.
Arthroscopy is extremely versatile and can address a wide range of shoulder conditions. While it cannot cure advanced arthritis, it is highly effective for issues involving tendons, ligaments, cartilage, and joint stability.
Below is a list of common problems arthroscopy can successfully treat:
Rotator Cuff Tears
One of the most common uses of arthroscopy. Surgeons can repair partial or full-thickness tears, remove inflamed tissue, and smooth bone spurs that contribute to cuff damage.
Labral Tears (e.g., SLAP lesions)
The labrum is a ring of cartilage that stabilises the shoulder. Arthroscopy allows surgeons to repair tears from injury, sport, or overuse.
Shoulder Impingement and Bursitis
Inflamed tissue or bone spurs can narrow the space in the shoulder, causing pain when lifting the arm. Arthroscopy can remove the irritants and improve function.
Recurrent Shoulder Dislocations
Arthroscopy can tighten or repair ligaments to prevent future instability episodes.
Frozen Shoulder (Adhesive Capsulitis)
When therapy alone hasn’t worked, arthroscopy can release the tight capsule restricting movement.
Cartilage Fraying or Minor Damage
Although it can’t reverse major arthritis, arthroscopy can smooth small areas of damaged cartilage to reduce pain.
Calcific Tendonitis
Calcium deposits within the rotator cuff can be removed arthroscopically with excellent outcomes.
AC Joint Problems
Arthroscopy can trim the end of the clavicle to relieve pain from arthritis in the acromioclavicular joint.
Arthroscopy is unlikely to be effective when there is:
In these cases, shoulder replacement is often the more effective and lasting solution for pain relief and function.
For the right patient, arthroscopy offers impressive and reliable outcomes. Here’s what you can expect:
1. Reduced Pain
Most patients experience major pain reduction once tissues heal and inflammation settles. Pain relief is often noticeable within weeks.
2. Faster Recovery
Because the incisions are small and tissue disruption is limited, the rehabilitation period is shorter than replacement surgery. Many patients resume light activities within a few weeks.
3. Improved Mobility and Strength
As repaired tissues heal and physiotherapy progresses, you’ll gradually regain range of motion and functional strength.
4. Preserved Natural Joint
You keep your original anatomy, which matters for long-term comfort, coordination, and athletic movement.
5. Lower Long-Term Risks
There is no artificial implant to loosen, wear out, or require revision.
6. Return to Sports or Work
Most people return to their sport, occupation, or hobbies once fully rehabilitated—especially after rotator cuff or labral repairs.
Here is a simple breakdown of why arthroscopy is often the better choice when appropriate:
Recovery varies depending on the repair required, but most patients can expect:
Your surgeon and physiotherapist will tailor a recovery program specifically for your condition and goals.
Although arthroscopy is highly effective in many situations, replacement is the better choice when:
In these cases, a joint replacement can restore comfort and function far more predictably.
Your care team will consider several factors:
Their aim is always to preserve your natural joint whenever possible—making arthroscopy the preferred option when the anatomy can be successfully repaired.
Shoulder arthroscopy is an excellent treatment for many common shoulder problems, particularly those involving tendons, ligaments, cartilage rings, and joint stability. When degeneration is minimal and soft-tissue damage is the main issue, arthroscopy often delivers outstanding outcomes with far less downtime compared to a full shoulder replacement.
However, when the joint is significantly worn or deformed, shoulder replacement becomes the more reliable choice for long-term pain relief and mobility.
If you’re unsure which option is right for you, speak with your surgeon and undergo appropriate imaging. With a clear diagnosis and a personalised plan, you can move forward with confidence—knowing the chosen treatment is the best fit for your shoulder and your lifestyle.